Finding a Lactation Consultant Near METhe San Francisco Bay Area is teeming with new life and vivre! It is no big surprise that we have a very high birth rate, given our population of childbearing workers and a bustling tech industry! We are a hub to Google, Facebook, Uber, LinkedIn, Apple, GAP and many other successful organizations!
Silicon Valley, SF and the East Bay all have their own care providers that specialize in the field of pregnancy, birth and postpartum. They work together collaboratively and individually to meet your needs. Having a baby for many people is a once in a lifetime event, and you deserve to have the best help that you can find! Here is a little summary of the issue that I wrote up for you, as you think about hiring a Midwife, Doula, or Lactation Consultant in the near future. 1.) You are pregnant or plan to be soon! Congratulations, you now have need of the services of someone experienced in childbirth and breastfeeding, non-pharmacological pain management during labor, childbirth classes, and breastfeeding classes, and lactation consults. 2.) Probably you are looking through lots of YELP profile pictures trying to pick a photo that resonates with your soul. A certain hairstyle, age or look is unlikely to be a useful focal point here. You most likely have used the Find a Lactation Consultant Near Me feature for google maps trying to see if that helps. Ultimately what assists many families is a proper information gathering search on a webpage versus using powers of divination! Some questions to ask yourself might be: What things are important to you? What is their vaccination status? A person’s background education in lactation or birth? What certifying body they trained with? How many years were they in practice for? What other families think of them? Whether they take a hands off approach? Trauma informed care? You have to think about what type of person you would like in your personal space and whether they will attend to your needs. 3.) Evaluate all of your alternatives for providers. Make a short list of what is very important, and just a little important to you. Think about what type of insurance coverage you have, and whether they have Lactation Consultants that are in-network. In the California Bay Area, some of the big players in the insurance world are United, Cigna, Hill Physicians, Aetna, Anthem, and Blue Shield of California. United and Cigna for the most part do not reimburse anything no matter what they tell you. You will have to use PAMF for Cigna and United or be willing to pay out of pocket. For Anthem, you can get a GAP extension for out of network coverage. For Hill Physicians I am in-network, but you will need to check with other providers individually. My suggestion is that you load up your FSA card so that you can hire an out of network LC if you have Kaiser. 3.) Make a short list of nearby Lactation Consultants. Now that you have made a list of possible candidates, think about the next step! How does a regular person evaluate a specialist for competency? I would suggest that they search for detailed reviews on YELP. Are they active locally near you? Has anyone wrote a good or bad review about them? Did they answer your email promptly? Did your Doctor know who they were? What have your friends that were successful said about having a lactation specialist, and what were their names? 4.) Search for a Connection. Did you read warmth from their voice or email interaction? What stands out to you on an emotional level or spiritual level? What is it that this person can offer you in particular outside of their clinical knowledge? Do you feel safer with this person in your corner? Now that you have thought about all of these things as part of your quest to have the best experience possible, let me remind you that your gut instinct is probably right. No matter how good someone seems on paper, they need to give you the right feeling. If they seem warm and you can imagine hanging out with them (and being comfortable), that is a good indicator that you might have the right fit. If you are interested in working with me you can find me at Bay Area Breastfeeding Support, I look forward to hearing from you! Warmly, Serena Meyer RN IBCLC
1 Comment
Erin's Story If your baby is on an extended nursing strike, the Internet can be a disheartening place. There are plenty of stories out there, but longer the strike, the more likely the story is to end with: "Unfortunately, little so-and-so never nursed again." This is not one of those stories. It took 40 days, but in the end, we made it from all bottles to all breastfeeding. It was Serena who coached us through. Without her guidance, I doubt we would have made it. Our strike started on September 15, 2016, when my son was just over 10 months old. I nursed him when he woke up, then gave him his solids for breakfast as usual. Toward the end of the meal, he began crying and pulling at his lower lip, and I saw he'd bitten it slightly. He calmed down quickly, and I thought nothing of it. A few hours later, I went to nurse him. He latched, sucked a few times, then pulled off, upset, and wouldn’t latch again. I pumped a feeding and gave it to him by bottle, then another, and another as he kept refusing to breastfeed. I figured he’d go back to nursing when his lip felt better. By the next day, however, he wouldn’t even try to latch when I offered. I’d always been home with him; the last time I'd pumped more than an occasional feeding had been just after my son was born, before we had tongue and lip ties released. I found myself struggling to keep up. I’d never had much fondness for my electric pump, so I was primarily using my hand pump. I’d offer a breast and then, when he refused, pump that feeding, no matter the time of day (or night). I had no freezer stash; I’d never needed it. I quickly began to worry about maintaining my supply, both to keep him fed and so there would be something for him to come back to. The following day, I took my son to the pediatrician to rule out any medical problems. Nothing. Good news, of course, but it also meant there was no obvious factor causing the strike that we could address. I tried to nurse him to sleep for a nap after the appointment — something he usually liked and sometimes even required — but he wouldn’t latch. I emailed a retired lactation consultant acquaintance, who replied with the words I’d feared: “nursing strike." I went straight to Google to read everything I could find about nursing strikes and how to end them. Most were said to last 2-5 days, maybe a week at the outer limit. We could make it until then, I thought. The following day, I started trying everything I could to get my son to nurse. I held him for a nap and offered as he woke up — no luck. We took a bath together, and I offered there — no luck. I offered after he was drowsy from his pre-bed bottle — no luck. He would snuggle up and happily take a bottle or suck his thumb, but he’d freak out if I so much as moved to offer a breast. I was shocked by how heartbreaking it was for me. I’d recently gone through a sudden divorce, moving cross-country and in with my parents, and the thought of what would quite possibly be my only baby, whom I'd planned to let self-wean, never nursing again was crushing. It felt so final; he was so adamant it freaked me out. I just kept thinking that the last time he’d nursed, I’d probably been browsing Facebook on my phone. I hadn’t even been paying attention. I swore if he’d come back, I’d never use my phone while nursing again. I told myself not to panic for at least a few more days; it was early still. The house I’d recently purchased was ready for us to move in, but I put off the move, afraid that making any major changes might prolong the strike. Instead, over the next days, I kept trying different ideas. I got my son to take one feeding from an open cup in case using a bottle was keeping him on strike, but by the second feeding, he’d had enough and refused. I tried to teach him to drink from a straw for the same reason, but he didn’t catch on. I got him a couple of learner cups, all of which he rejected. I switched to a slow-flow nipple instead of the “age-appropriate” one we’d been using. We did skin-to-skin when we could, but it was hard while sharing a living space with others. One time, he started to latch before pulling away. Another time, he bit rather than latching. He fell asleep with a bottle, and it broke my heart that he was so comfortable with that imposter breast. I rocked him to sleep with the breast nearest his face out. We tried different positions and places to no avail. I called the lactation consultant associated with our pediatrician’s office, but she didn’t have any more ideas. I noticed he seemed to be pigging out on solids, eating way more than he had been even a few days earlier, and I got worried I wasn’t producing enough milk for him. I rented a Medela Symphony and started power pumping. I even managed to get a feeding ahead. I posted in several Facebook groups, including Serena’s, looking for advice. Through one of these groups, a mom with a similarly aged baby who was also on strike contacted me, and we struck (no pun intended) up a kind of friendship, brought together by the strange and stressful situation we found ourselves sharing. It helped immensely having someone to talk to who knew what this felt like. A week into the strike, I noticed something white on the inside of my son’s top lip. It looked a bit like blisters to me. Someone said thrush; someone else suggested hand, foot, & mouth. Back to the pediatrician we went, where we figured out the lip was torn up from the shape of the bottle we’d been using, the friction of teeth against lip against bottle wearing tooth-shaped patches. He didn't seem to be in pain, but the doctor warned I would need to switch to a faster flow bottle soon to avoid things getting worse. I went out and bought another brand of bottle, hoping a different nipple shape would alleviate the problem, and it seemed to help. A couple of days later, my son started letting me express milk into his mouth now and then, which I hoped was a good sign, and occasionally he’d let the very tip of a nipple touch his lip. It didn’t feel like much progress, though. I reached out to local LLLI leaders who, though kind, didn’t have any more ideas for me to try. I knew the people around me were wondering why I didn’t throw in the towel, especially given everything else we were dealing with. But in a way, it was because of all that that I needed to keep going with what I believed was right for us. I needed us to beat this thing. Thirteen days into the strike, I talked to Serena. She had me send a video of me offering to nurse my son and immediately labeled his refusal as behavioral, not caused by pain or discomfort. Though the strike may have started from mouth pain, in the days that followed he had decided not to nurse, that he preferred a bottle. She had a plan, and I was so relieved to feel like I was taking actual steps toward a resolution. Serena had several suggestions right off the bat. She wanted me to focus on increasing my supply so that I was pumping several ounces more than what my son was eating each day. That way, there would be plenty of milk ready and waiting if/when he decided to latch, not to mention a little bit of a freezer stash just in case. We were to switch gradually from our current bottles (Avent Natural) to Dr. Brown’s, starting with a faster flow nipple and moving to progressively slower ones every few feedings until we were using preemie nipples. I stopped offering to nurse. Instead, I gave my son his bottle in nursing position, with the bottle held in my armpit, and gradually worked on having the corresponding breast out during the feeding. As he got more comfortable, I started holding the back of his head as I always had to help him latch, making sure he could see the bottle as I did so to keep him from thinking I was going to make him nurse. Soon enough, he was comfortable taking his bottle like he was breastfeeding, breast out and everything -- though he would look around for the bottle to make sure it was there. It was around this time that I decided to move into the new house. Maintaining the status quo wasn't breaking the strike, so perhaps novelty would. We would have less practical support after the move, but there would be more baby-friendly areas where I could let my son play while I pumped, and with our own space, walking around topless (another common piece of strike advice!) was actually possible (not that it helped in our case). After a few days of “armpit boob,” Serena gave us the ok to try using a nipple shield, which would feel more like a bottle nipple to my son. I tried taking the bottle away mid-feeding and offering a breast with a shield full of expressed milk and a letdown I’d stimulated with a hand pump. He got upset and refused, but I suspected it was more at having his feeding interrupted than about the breast itself. We finished the feeding by bottle. A couple of times he fell asleep with the bottle for a nap, and I’d offer a breast with the shield when he woke up. Both times, he just cried until he found his thumb. I even tried offering once in the middle of the night after I’d rocked him back to sleep, but he didn’t even acknowledge that I was tickling his lip with a nipple shield. He never was a dream feeder, and if he wanted to suck, he’d find his thumb. On day 20, I got my son to latch twice with a full shield. He gave a few sucks each time before pulling away and refusing to try again. The third time I tried, he flat-out refused. Serena reassured me that it was progress and that the process might take weeks. When I asked her to tell me when it was time to be discouraged, she replied: "I am never discouraged because all things are possible." The next day, my son nursed twice, and I was ecstatic. We used the shield, and I had to do breast compressions the whole time, but he nursed! It seemed miraculous. The biggest issue was that he was biting like crazy. He’d go to latch, then clamp down on my nipple for what felt like an eternity before finally relaxing into nursing. Without the shield as a kind of buffer, I’m not sure our efforts would’ve been sustainable. He was biting all kinds of things at the time — furniture, my legs, stuffed animals — so I wondered if maybe he was teething or something. I tried ibuprofen the next day, but it didn’t seem to lessen the biting. We did get a couple more nursing sessions in, with lots more biting. He started opening his mouth to relatch after letting go mid-feeding instead of sucking his thumb, which was a tiny step in the right direction. When he refused to breastfeed, or when my nipples were too sore to try, we’d do a bottle. I started to worry that continuing to let him bite and not unlatching him when he did (since waiting out the bite was the only way to get him nursing) would turn into a habit. After a few days of letting him bite, I started taking him off each time he clamped down. I’d offer an ounce of milk by bottle, then try to latch again. That didn’t work, and I was afraid he'd either develop negative associations with the nipple shield if I kept offering and then removing him or decide biting was a way to get a bottle. We went back to bottles full time. It felt like such a setback, coming on the heels of what has seemed like great progress. I reached out to everyone I could think of about the biting, but no one had ideas beyond teething. I think by this point, most people I knew thought I was well and truly crazy for not having given up by now. But still, I just couldn’t. I knew I wasn’t ready to be done breastfeeding, and I believed my son wasn’t, either. After a few days’ break, I offered a breast without the shield, just to see what would happen. My son started to latch, then bit me. I tried giving half-feeding bottles to take the edge off of his hunger, then offering with a shield. He wasn’t having it. Serena advised us to go back to armpit boob for a day so that he didn’t start rejecting breastfeeding altogether. "Go slower," she said. I was afraid each feeding by bottle would carry us further away from breastfeeding, but Serena's logic made sense. Four weeks into the strike, I had to cancel plans I'd been looking forward to for reasons unrelated to the strike. With that disappointment added to the discouragement of the past few days, I was feeling particularly low. It was a beautiful fall day, unseasonably warm, so I decided to take my son out into the backyard. We sat together on a blanket, looking at birds and leaves and reading books together. It felt like a connection that had been strained during the strike was strengthened. At one point, when I had him on my lap, he turned toward me and almost rooted for a breast. Back inside, we put on some music and danced around our living room together, something he loved. Then I donned the shield and offered…and he latched without biting! It was evening, and my supply was low, so there wasn’t much milk at the ready. He quickly became frustrated and let go. But oh, it was progress. The next day, day 29, my son nursed once in the morning, using the shield but without biting. I was ecstatic. The second feeding, though, he played around and then bit. Serena told me to slow down. She assigned us one week of only trying to nurse for the first feeding of the day, with the shield, and doing the rest by bottle. After five days of successful single morning nursing sessions, Serena let us go up to two nursing sessions a day. At first the second one was iffy, but after a couple of days it became routine. On day 40, after a week of successfully nursing twice a day and doing the rest of the feedings by bottle, Serena bumped us up to four feedings. They went so well the first day that she told me to pull all bottles and see what happened. He kept nursing! That first bedtime nursing in six weeks, he went for a whole hour, like he was reveling in this familiar ritual we’d almost lost. I was reveling, too. He was a different baby — taking his time, playing, stopping to babble or look around — but he was breastfeeding. And it made sense. It had been a month and a half, and he was more like a toddler now at almost a year old than the baby he’d been when the strike began. He now got excited when he saw the hand pump I still used to stimulate letdown, like he used to get excited when he saw a bottle, and the change made me so happy. The road was not completely smooth from then on. At times, it was like he had forgotten how to nurse. He’d latch happily, then lie there for 30 or 40 minutes not really sucking. Several times he bumped his mouth while playing, and I went into complete panic mode, terrified he would go back on strike from the pain. The biting came back sometimes, a hard, long, clamping chomp that he used on breast and toy and furniture alike. I continued to pump, first to decrease the oversupply I’d intentionally built during the strike and then to supplement what he was getting from breastfeeding, as I suspected he continued to struggle. There was a period a few weeks after the strike ended that we were back down to a single breastfeeding session per day; the rest of his feedings he took by straw cup after refusing a breast. Finally, I contacted a local craniosacral therapist about the biting, which I suspected was somehow linked to the ongoing breastfeeding challenges. My son had had problems with face and neck tension that had affected his latch around five months of age, which we’d resolved with the help of a CST where we lived at the time. The new one we saw took one look at my son, tried to do one short exercise with his mouth (which led to him crying and cowering away from her for the remaining 45 minutes of the session), and referred us to a feeding therapist. This, it turned out, was exactly what my son needed. Over the months since, through weekly sessions and daily exercises that we do at home, he has gradually released a huge amount of tension from his jaw and face and developed movement patterns and muscles that allow him to nurse comfortably as well as eat solids and drink from a straw so much more effectively. The difference is staggering; it's easy to see how much wider he can open his mouth and how much better he can manage food as he chews, not to mention the improvement in breastfeeding. I have not pumped since a month into therapy. And according to our therapist, uncovering and working on these issues now will avert food aversions and even speech problems down the road. I don’t believe it was these issues that caused the strike in the first place, but I do believe they made it harder for us to get back on track, especially once the strike was over. They also explain why, months before the strike began, the Baby-Led Weaning approach to introducing solids was a spectacular failure for us. My son is now 16 months old. Our breastfeeding looks different from what it did before the strike, and not just because he's older. We still use a shield; the one time I tried without it, he bit me. He also stopped asking to nurse when the strike began, and he has never started again. I offer five times a day, based on when he wakes up, naps, and goes to bed on a particular day, and that seems to work for us. And nice as that first hour-long bedtime session was, he has since cut back to a more manageable 10-15 minutes most of the time. Oh, and my promise not to use my phone while breastfeeding? Still going strong. Some things are too precious to miss, and it took losing one of them for a time for me to realize that. Welcome to my Clinical Lactation Support blog. I like to tuck away some of my thoughts and treatments Ideas here.
Mastitis is associated with a fever over 100.4 and a red area on the breast that is very painful. Because of the associated fever keep replacing fluids and supporting immune system health. You can treat a fever with either Ibuprofen or Tylenol safely while breastfeeding. Start dose of ibuprofen at 800, then once fever is down, can alternate Tylenol and ibuprofen at much lower doses until pain and infection is resolved. Ibuprofen every 8 hours (400 mg- 800 mg). Good to keep the max dose over 24 hours at or under 3000mg Tylenol every 4-6 (325 mg-650 mg). Good to keep the max dose over 24 hours at or under 3000mg If your fever is still high when using one of these, you can take both types of medications at once if needed. Watch your top maximum dose over 24 hours with Tylenol in particular since it is metabolized in the liver. A single dose should not go over 650 every 4-5 hours at the highest. Do not take the ibuprofen on an empty stomach. Please contact your primary healthcare provider if you have a sustained temp over 100.4 it is likely time to add in one of these antibiotics. All are compatable with breastfeeding. There is a fantastic evidence based article available that says this: Nursing mothersOutpatient treatment Outpatient options includes the following:
Full Article here: http://emedicine.medscape.com/article/2028354-overview For a more holistic treatment of mastitis you will want to use vigorous massage prior to breastfeeding with a oil carrier of at least I teaspoon to one drop of essential lavender oil, and a breast poultice of sliced or grated potato placed directly on the breast. Heat the breast before breastfeeding and cool it down afterwards. There is good evidence cited here: http://cid.oxfordjournals.org/content/50/12/1551.full that says treatment with probiotics L. fermentum CECT5716 or L. salivarius CECT5713 will help resolve mastitis. The key probiotic strains are sold, but not together. I looked for a bottle that had both but I could not find one. http://www.swansonvitamins.com/swanson-ultra-femflora-feminine-probiotic-formula-60-caps and this one: http://www.swansonvitamins.com/swanson-probiotics-dr-stephen-langers-ultimate-16-strain-probioticwith-fos-60-veg-caps Take both of these each day along with 4800mg of sunflower lecithin to prevent any future blocked ducts. So lets start with those, add garlic into your diet for immune system support, make sure you are eating enough iron rich foods, and also consider a dilute amount of oil of Oregano. Be sure that you never offer an Essential oil to a baby. Consider reading over my article on mastitis: http://nativemothering.com/2011/10/what-are-some-of-the-predictors-and-solutions-for-mastitis/ -Serena Meyer RN IBCLC THE “ALL-PURPOSE NIPPLE OINTMENT” OR APNO
We call our nipple ointment “all purpose” since it contains ingredients that help deal with multiple causes or aggravating factors of sore nipples. Breastfeeding parents with sore nipples don’t have time to try out different treatments that may or may not work, so we have combined various treatments in one ointment. Of course, preventing sore nipples in the first place is the best treatment and adjusting how the baby takes the breast can do more than anything to decrease and eliminate the breastfeeding parent’s nipple soreness. Please note that the “all-purpose nipple ointment” is a stop gap measure only and that the definitive treatment of sore nipples is to help the baby latch on as well as possible. See these other information sheets: Sore Nipples, Latching and Feeding Management. THE APNO CONTAINS:
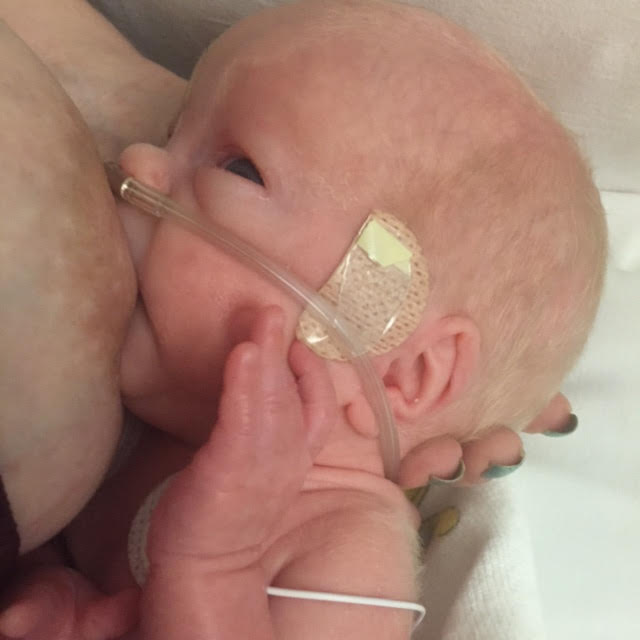
Note that nystatin ointment, which we used to use and which decreases the concentration of the other ingredients, is far inferior to miconazole and also tastes bad. I write the prescription this way. 1. Mupirocin ointment 2%: 15 grams 2. Betamethasone ointment 0.1%: 15 grams 3. To which is added miconazole powder to a concentration of 2% miconazole Total: about 30 grams combinedApply sparingly after each feeding. Do not wash or wipe off. NO SUBSTITUTIONS If possible, it is best to get the prescription filled at a compounding pharmacy. You can find a list of compounding pharmacies by going to http://www.pccarx.com/. Click “Find a compounder” at the top, then add relevant information. HOW TO USE THE OINTMENT: 1. Apply sparingly after each feeding. “Sparingly” means that the quantity of the ointment used is just enough to make the nipples and areola glossy or shiny. 2. Do not wash it off or wipe it off, even if the baby comes back to the breast earlier than expected. HOW LONG SHOULD THE OINTMENT BE USED? Any drug should be used for the shortest period of time necessary and the same is true for our ointment. If the breastfeeding parent still needs the ointment after two or three weeks, or the pain returns after the breastfeeding parent has stopped the ointment, the parent should get “hands on” help again to find out why the ointment is still necessary. The most important step for decreasing nipple pain is still getting the “best latch possible.” Sometimes a tongue tie has not been noticed and is a reason for continued pain. Some pharmacists have told breastfeeding parents that the steroid in the ointment will cause thinning of the skin if used for too long. While this is a concern with any steroid applied to the skin, we have not seen this happen even when breastfeeding parents have used it for months. Updated February 2017 The information presented here is general and not a substitute for personalized treatment from an International Board Certified Lactation Consultant (IBCLC) or other qualified medical professionals. This information sheet may be copied and distributed without further permission on the condition that it is not used in any context that violates the WHO International Code on the Marketing of Breastmilk Substitutes (1981) and subsequent World Health Assembly resolutions. If you don’t know what this means, please email us to ask! Questions or concerns? Email Dr. Jack Newman (read the page carefully, and answer the listed questions). Make an appointment at the Newman Breastfeeding Clinic. The uncertain journey of a preemie is hard to cope with. Nicu life is full of ups and downs that are almost indescribable. The joy you feel when your little one goes up an ounce, the pain you feel every time you walk back to your car to head home without your child. In a world that can feel so helpless, I find some within support and encouragement of others. I knew Liam was going to most likely come early, but not this early. At 21 weeks I got and iugr diagnosis. Then at 28 weeks preeclampsia set in. I thought all the reading, support groups online, and googling everything I could about preemies would prepare me, but nothing prepares you for your child being born months early at just a pound and a half. There wasn't much I could do, except focus on being the best mom I could. I started pumping that night, bringing little bullets with a few drops over to the nicu. My supply came in quick this time, even if it isn't abundant. In a time where I wasn't even able to hold my child till he was 4 days old, providing milk was something I could be proud of. I follow posts from other moms in hopes I will gain some knowledge for when the time comes for Liam to drink from my breast, rather than the tube he gets fed through. Last week we hit 3 lbs and at 32 weeks, breastfeeding gets brought up. It's been days of hoping that I'll be able to try. Waiting for those cues. Waiting for one of the nurses to feel comfortable with him trying. Today was that day. He did so well. With tubes, sensors, and wires everywhere, it still felt so natural. He was even able to get a latch and a suck a few times. 7 weeks away from the day he's supposed to be born, he knows just what to do. It makes me believe that there's nothing more natural and nothing more beautiful. Even though we had to wait 5 weeks, I'm so grateful I get to go through this new part of his journey with him. -Natalie Murray PREVENTION OF SORE NIPPLES: To prevent sore nipples, ensure a large amount of areola enters baby’s mouth! Do not coat a thrush infected nipple with expressed milk for healing- it actually feeds the yeast and makes it worse. A simple rinse will do.
PROBIOTICS: You want the fancy “Women’s Health Probiotics” .hese are for the mother to take. THRUSH: TREATMENT OF Candida Infection NIPPLES will need the care of your OBGYN for APNO ointment for signs of Thrush. Wipe off excess. The following link is a sheet to print out for your Dr. http://www.breastfeedinginc.ca/content.php?pagename=doc-APNO but if that link is not working you can link my directions for healthcare providers for APNO found on my blog. This will have dosing directions but typically you apply a thin sheen over the nipple and areola each time after nursing. This means use a ½ pea sized amount and rub your fingers together until it disappears, then use it on your nipples. In this amount it is compatable with breastfeeding. If the APNO does not resolve the thrush alone: “Persistent Pain” Academy of Breastfeeding Medicine 2016, "Oral fluconazole (200 mg once, then 100 mg daily for 7–10 days) may be used for resistant cases. Before prescribing fluconazole, review all maternal medications and assess for drug interactions. Do not use fluconazole in combination with domperidone or erythromycin due to concern of prolonged QT intervals.” Evidence of Pediatric Thrush: If the Baby has a small amount of light white on the tongue that will not wipe off, Contact the Pediatrician so the infant and the mother get concurrent treatment and do not pass it back and forth. Remember the goal with oral nystatin is to paint the inside of the babies mouth, vs put it alongside one cheek just to be swallowed. Spread it around! LAUNDRY: when you have thrush will need Grapefruit seed extract and it into your wash to help kill candida on clothes. Dry on hot, or sun dry. Bleach if you need to. Be aware that anything that touches your breast may hold onto the spores, so separate the towels; you get your own. Boil things that go into your baby’s mouth or steam them in a sterilizer bag (Bottle nipples, chewwies, pacis, pump flanges) I think a steamer bag is easier than boiling everything. Please carefully reconsider the instructions from anyone to apply grapefruit seed extract to your nipple neat- it is a great way to chemically burn your nipple. CANDEX: Candex is a small tablet that slow down cellular division of candida. Its great for adults with chronic overgrowth of candida (Thrush) It's compatible with breastfeeding/chestfeeding. The Thrush Plan:
Serena Meyer, RN, IBCLC, RLC Preparing for Your Return to Work: The Breastfeeding Mother’s Guide
When a family is expecting a baby, it’s a time full of wonder and happy expectation. For months, a mother feels fluttering and quickening, the soft movements of her baby. For many families, it is also a time for making plans to welcome a new family member. Parents may also use the time of pregnancy or the waiting period for adoption to investigate how to support the breastfeeding relationship in the workplace or in school. This article addresses some common questions breastfeeding mothers have about preparing for a return to work and includes the concerns that mothers who do not have a pro-breastfeeding workplace or school may face. Talk to your employer This article, Pumping 9 to 5, provides some information on how to talk to your employer about breastfeeding and how to make a plan for expressing your milk at work. Being ready for this conversation, with an idea of what you will need in terms of space and time, will help make your points clear and concise. Take the time you need to make a plan before you speak with anyone at your school or job. Other workplaces, tribes, and many places of higher education have set up lactation rooms; think about bringing them up in your conversation to support your requests. It may also be important to mention the ways your workplace or school will benefit from setting up a lactation room for other families. This booklet explains some of the possible concerns that a business or institution may have about setting up a lactation program for individuals that either work in or attend the facility. Know your rights There are State and Federal Laws in place to support breastfeeding mothers. For example California Labor Code 1030-1033 stipulates: Every employer, including the state and any political subdivision, shall provide a reasonable amount of break time to accommodate an employee desiring to express breast milk for the employee's infant child. The break time shall, if possible, run concurrently with any break time already provided to the employee. Additionally, the IHS and many Government agencies provide pumping breaks for their employees, and many institutions already have supportive programs in place for breastfeeding mothers. The Affordable Care Act of 2010, states that: Effective March 23, 2010, the Patient Protection and Affordable Care Act amended the FLSA to require employers to provide a nursing mother reasonable break time to express breast milk after the birth of her child. The amendment also requires that employers provide a place for an employee to express breast milk. Consider all of your options Are you able to change your work schedule or delay returning to work or school? Some mothers have worked out job shares or found other ways to minimize separation from their babies. Talk to your employer about what might work for you.
When should I start expressing milk? Babies grow so fast! They are newborns for only a few weeks, and before you know it, they are smiling, cooing, and reaching for your face while you are nursing. In the first several weeks after birth, take all the time you can to relax, get to know your baby, and just enjoy being his mom. Unless you have to return to work right away, it is recommended that mothers wait until breastfeeding is well-established before they begin expressing milk for returning to work: for most mothers, somewhere between 3-4 weeks. If you have to return to work earlier than 4-6 weeks, you might wish to begin pumping milk two weeks before you plan to return to work. Learn how to express your milk Preparing for your return to work or school can begin with learning to express your milk.
How do I hand express? Hand expression requires no special equipment and can be an effective way for you to remove milk when separated from your baby. Some mothers find that hand expression is more effective for them than pumping because it is more comfortable, and they can feel for areas of fullness and apply pressure with their fingers exactly where it is needed. Once you have success with a method of hand expression, you may feel that you are able to meet your baby’s needs without a pump. What type of pump should I use? A high-quality, full-size, double-electric pump is recommended for a mom who plans to pump milk every day. A pump that is made by a manufacturer specializing in breastfeeding equipment will be of higher quality than cheaper pumps made by a company whose primary products are bottle-feeding equipment or baby food. A breast pump is an item for which the old adage, “You get what you pay for,” often rings true. Another option for many mothers is renting a multiple-user pump from a trusted source such as a Hospital, Tribal Health Clinic, or local IBCLC. Most WIC offices provide pumps to moms who are returning to work or school; contact your local WIC office to see if you qualify. Many families have health insurance that is willing to cover the cost of renting a hospital-grade pump. If you are able, call your insurance provider for the details of your own coverage when you are pregnant. Recent 2011 news from the IRS states that electric pumps are now tax deductible, so keep your receipts for your tax records. In our opinion, the top three single user pumps on the market today are: Pump Brand/Model Cost range Warranty Mechanics WHO-CODE Spectra S1 or S2 $115-250 2 year Closed system Compliant Hygeia Enjoye* $180-300 3 year Closed system Compliant Ameda Purely Yours $150-180 1 year Closed system Compliant Medela Pump in Style $250-350 1 year Open system Non-compliant *Sold in the category commonly referred to as single-user pumps; Hygeia is the only pump company that has sought and received FDA approval for their pump to be used by more than one person. What is the difference between an open and closed system pump?
What is the WHO CODE, and why is it important to consider when buying a breast pump? The “WHO CODE” is short for the World Health Organization’s International Code of the Marketing of Breastmilk Substitutes. Part of the purpose of the WHO CODE is to protect breastfeeding by preventing aggressive marketing of breastmilk substitutes and artificial nipples. Many people prefer to purchase a breast pump from a company that is supportive of and compliant with the WHO CODE. More information on both the breast pumps, the WHO CODE, and open and closed systems can be found at: The Problems with Medela How often should I express milk? Once a day is usually plenty at the beginning. Most moms find that they are able to express the most milk in the morning hours. You can nurse your baby on one side while expressing milk on the other side. Or you could pump both sides about one hour after your baby’s first morning feeding. Don’t worry if you don’t get very much milk at first. It takes practice, and your body needs to “learn” to make milk for that extra “feeding.” When milk is removed, your body responds by making more milk at a faster rate. It can take a few days for your body to increase production (Daly, Kent, Owens et al.,1996). Any milk collected during these practice sessions can be stored in the freezer. How much milk should I have stored in my freezer? Many mothers find that they feel less stress if they to know that they don't need to create a large freezer stash of milk before they return to work. Instead, they can use their maternity leave to focus on being with their babies and getting breastfeeding well-established. If you have enough milk to send with your baby on your first day, then you have enough in the freezer. It is important to express as much milk while you are at work as your baby needs during that time. If your baby needs 10 ounces while you are away at work, then you need to pump at least 10 ounces each day. For example: If you were to only pump 8 ounces and send 2 ounces from the freezer each day, you would not be expressing the amount of milk your baby requires. Your body will “think” that your baby needs 2 fewer ounces each day than he really does, and your production will not match his demand. If you start to run out of milk in your freezer, you may face the difficult decision of how to meet your baby’s needs. Many mothers learn too late that increasing their milk supply to meet their baby’s demands is more complex than it seems. Meeting your child’s daily needs for expressed milk during separation is the best way to avoid difficulties later. Using the simple system described, you pump each day what your baby would need the next day. This way you only use the small freezer stash for emergencies, such as dropping and spilling a day’s worth of milk, or other milk-related calamities. If you need information about returning to work or expressing your milk, a Breastfeeding Counselor , La Leche League Leader, Nursing Mother’s Counsel or International Board Certified Lactation Consultant may be able to help. Accessing a community support system can help you reach your breastfeeding goals. You may also be interested in these articles: Returning to Work: The Breastfeeding Mother’s Guide Are There Differences Between Breastfeeding Directly and Bottle-Feeding Expressed Milk? Breast versus Bottle: How Much Should Baby Take? Facts Every Employed Breastfeeding Mother Needs to Know I’m Worried My Milk supply is Drying Up, What Can I Do? References Black Bear, J. (2011). Breastmilk Storage and Handling Guidelines. http://nativemothering.com/2011/04/breastmilk-storage-guidelines/ Daly, S., Kent, J., Owens, R. & Hartmann, P. (1996). Frequency and degree of milk removal and the short-term control of human milk synthesis. Exp Physiol, 81(5), 861-75. Easy Steps to Supporting Breastfeeding Employees. (2008). U.S. Department of Health and Human Services, Health Resources and Services Administration (HRSA), Maternal and Child Health Bureau. Produced in contract with Every Mother, Inc. and Rich Winter Design and Multimedia. http://mchb.hrsa.gov/pregnancyandbeyond/breastfeeding/easysteps.pdf Forbes, B. (2011). What is the WHO-CODE? Website: http://www.bestforbabes.org/what-is-the-who-code Internal Revenue Bulletin. Lactation Expenses as Medical Expenses. (2011). Website: http://www.irs.gov/irb/2011-09_IRB/ar11.html Jones E., Dimmock, P. W. & Spencer, S. A. ( 2001). A Randomised Controlled Trial to Compare Methods of Milk Expression After Preterm Delivery. Arch Dis Child Fetal Neonatal Ed, 85, F91–F95 Meier, P. Engstrom, J. Janes, J. Jegier, B. & Loera, F. (2012). Breast pump suction patterns that mimic the human infant during breastfeeding: greater milk output in less time spent pumping for breast pump-dependent mothers with premature infants. Journal of Perinatology, 32, 103-110 Morton J., Hall, J., Wong, R., Thairu, L., Benitz, W. & Rhine, W. (2009) Combining hand techniques with electric pumping increases milk production in mothers of preterm infants. Journal of Perinatology, advance online publication,29, 757-764 Shebala, M. (2012, January 26). Benefits of breastfeeding in workplaces touted. Navajo Times, http://www.navajotimes.com/opinions/2012/0112/012612notebook.php Silver, B. (2010). College and University Lactation Programs, some Additional Considerations. The Elsevier Foundation, University of Rhode Island Schmidt Labor Research Center.http://www.uri.edu/worklife/family/family%20pics-docs/LactationPrograms%20FINAL.pdf Simmance, A. (2011). Why You Shouldn't Buy, Sell, or Borrow a Second Hand Medela Swing Pump. Website: http://mythnomore.blogspot.com/2011/08/why-you-shouldnt-buy-sell-or-borrow.html State of California, California Labor Code § 1030. 2002: Chapter 3.8, Section 1030, Part 3 of Division 2 of the Labor Code http://www.google.com/url?q=http%3A%2F%2Fwww.cdph.ca.gov%2FHealthInfo%2Fhealthyliving%2Fchildfamily%2FPages%2FCaliforniaLawsRelatedtoBreastfeeding.aspx%23workingandbreastfeeding&sa=D&sntz=1&usg=AFQjCNHUWIwkLISI2im9IiolxL9ZB-IVhA West, A. (2011). The Problems with Medela. Website: http://www.justwestofcrunchy.com/2011/01/19/the-problems-with-medela/ © 2012 Serena Meyer, IBCLC and Teglene Ryan, IBCLC |
Details
Authors
Archives
July 2023
Categories |
Chat
×
Connecting

You:
::content::
::agent_name::
::content::
::content::
::content::


 RSS Feed
RSS Feed